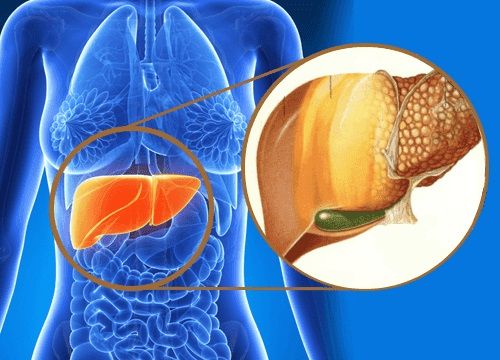
What is the fatty liver?
Fatty liver or hepatic steatosis is an accumulation of fat in the liver that causes inflammation and destruction. This process if not interrupted can cause fibrosis to appear and over the years 20% may end up in liver cirrhosis and 2% liver cancer
Causes of fatty liver
The frequent causes that generate a fatty liver are:
-
- Obesity / overweight: a person is considered obese if their body mass index (BMI) is calculated by dividing the weight by the height in cm squared: for example for a person of 85 kg and 1.70 m the BMI: 1.70 × 1.70 = 2.89, 85 / 2.89 = 29.4) is greater than or equal to 30. Between 29.9 and 25 is considered overweight and below 25, normal.
- Alcohol: there is a risk of liver damage with a daily alcohol intake of 20-25 grams (women) or 35-40 grams (men). If the daily consumption of alcohol exceeds 60 grams for more than 5 years, cirrhosis develops. As an example, a beer cane contains 8.8 grams of alcohol, a glass of wine of 12 to 14.4 grams (depending on whether it is white or red) and a whiskey or rum or gin, 19.2 grams of alcohol.
- Increase in cholesterol and triglycerides.
- Increased glucose (type 2 diabetes and insulin resistance).
- Medications: amiodarone (to combat ventricular arrhythmias), antiretrovirals, glucocorticoids and estrogens, diltiazem (vasodilator), etc. They should be discontinued in case of fatty liver.
Difference between a healthy liver and a fatty one
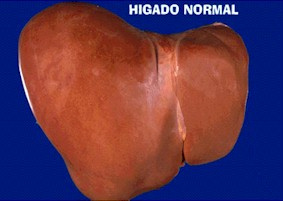
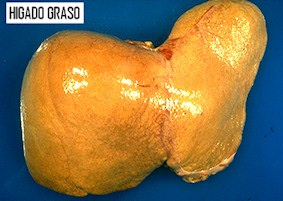
The fatty liver is the second cause of liver transplantation in the US.
Diagnosis
Fatty liver can be diagnosed by a blood test (transaminases) and the ultrasound technique (ultrasound) or a liver biopsy. It is important to note that most patients do not have symptoms because they have fatty liver.
In ultrasound, it is diagnosed by increasing the contrast of the liver in relation to the kidney. It should be noted that ultrasound, despite being a very reliable tool for the diagnosis of fatty liver, is not capable of diagnosing it in all cases. Other methods available are magnetic resonance, etc.


Fatty liver treatment
There are a number of drugs that are useful for eliminating liver fat, interrupting inflammation and destruction: ursodeoxycholic acid, pentoxifylline, vitamin E, metabolic corrections, pioglitazone, etc. It must be borne in mind that the treatment to completely eliminate liver fat and prevent the progression of the disease can last for months or even years. For this reason, in case of fatty liver, you should go regularly to the hepatologist to review the evolution and possible increase in dose of drugs or change them. In relation to the specific causes of fatty liver:


Alcohol: It is imperative that the patient completely suppress alcohol intake (whatever the cause of fatty liver).
Cholesterol, triglycerides: The patient must make a low-fat diet (which will be given to him by his hepatologist) and must also receive specific drugs to normalize cholesterol and triglyceride values (eg, statins).


Glucose: The patient must make a diet low in carbohydrates and exercise (at least 3 hours per week). Your hepatologist can prescribe drugs to lower blood glucose (oral antidiabetics, insulin).
Medications: The corresponding drug should be discontinued and replaced by similar ones that do not produce fatty liver.
The Hepatitis Viral Study Foundation Clinic is a pioneer center in offering the revolutionary PNPLA3 genetic test, being a result of its research work.
How the evolution of fatty liver can be predicted
- Homozygous CC: no risk of progression of liver damage.
- Heterozygous CG: with risk of progression to more severe forms of liver damage (increased liver fibrosis)
- Homozygous GG: with risk of progression to more severe forms of liver damage (increased liver fibrosis)
References
- Chalasani N, et al. The diagnosis and management of non-alcoholic fatty liver disease: practice guideline by the American Association for the Study of Liver Diseases, American College of Gastroenterology, and the American Gastroenterological Association. Hepatology 2012;55:2005-23.
- Neuman MG, et al. Alcoholic and non-alcoholic steatohepatitis. Exp Mol Pathol 2014;97:492-510.
- Yeh MM, Brunt EM2. Pathological features of fatty liver disease. Gastroenterology 2014;147:754-64.
- Rotman Y, et al. The association of genetic variability in Patatin-Like Phospholipase Domain-Containing Protein 3 (PNPLA3) with histological severity of nonalcoholic fatty liver disease. Hepatology 2010;52:894-903.
- Singal AG, et al. The effect of PNPLA3 on fibrosis progression and development of hepatocellular carcinoma: a meta-analysis. Am J Gastroenterol. 2014;109:325-34.

Consult our doctor
Dr. Vicente Carreño
Hepatology specialist
REQUEST INFORMATION WITHOUT COMMITMENT

Autoimmune hepatitis
It is a progressive chronic inflammatory disease of the liver that can lead to liver cirrhosis.

Hepatitis B
It is a viral infection of the liver that causes inflammation of the liver and the death of hepatocytes.

Hepatitis C
Hepatitis is an inflammation of the liver, and in the case of hepatitis C, caused by infection with hepatitis C virus (HCV)

Hepatitis E
Hepatitis E is an acute inflammatory disease of the liver that can lead to fulminant hepatitis.

Hidden infection by C virus
Up to 30% of patients with cryptogenic hepatitis can be caused by the seronegative hidden infection by hepatitis C virus (HIC).

Cholangitis
It is a chronic progressive liver disease that mainly affects women (90% of cases) from the fourth decade of life.